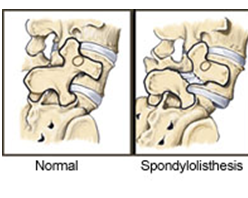
 SPONDYLOLISTHESIS - occurs when one vertebra slips forward on the adjacent vertebrae. This may produce a gradual deformity of the lower spine and also a narrowing of the vertebral canal or the exit points of the spinal nerves. If abnormal motion allows this vertebra to slip back and forth spinal nerves may be affected causing pain, numbness, tingling or weakness in the legs. Many individuals do not have symptoms with this condition while others experience long standing back pain.
SPONDYLOLISTHESIS - occurs when one vertebra slips forward on the adjacent vertebrae. This may produce a gradual deformity of the lower spine and also a narrowing of the vertebral canal or the exit points of the spinal nerves. If abnormal motion allows this vertebra to slip back and forth spinal nerves may be affected causing pain, numbness, tingling or weakness in the legs. Many individuals do not have symptoms with this condition while others experience long standing back pain.
There are five major types of spondylolisthesis:
Type I
Type I is called dysplastic spondylolisthesis and is secondary to a congenital defect of either the superior sacral or inferior L5 facets or both with gradual slipping of the L5 vertebra.
Type II
Type II is called isthmic or spondylolytic and is where the lesion is in the isthmus or pars interarticularis. This has the greatest clinical importance in persons under the age of 50. If a defect in the pars interarticularis can be identified but no slipping has occurred, the condition is termed spondylolysis. If one vertebra has slipped forward on the other (horizontal translation), it is referred to as spondylolisthesis.
Type II can be divided into three subcategories:
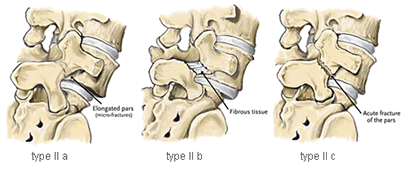
- Type II A – is sometimes called lytic or stress spondylolisthesis and is most likely caused by recurrent micro-fractures caused by hyperextension. It is also called a “stress fracture” of the pars interarticularii and is much more common in males.
- Type II B – probably also occurs from micro-fractures in the pars. However, in contrast to type II A, the pars interarticularii remain intact but stretched out as the fractures fill in with new bone.
- Type II C – is very rare in occurrence and is caused by an acute fracture of the pars. Nuclear imaging may be needed to establish diagnosis.
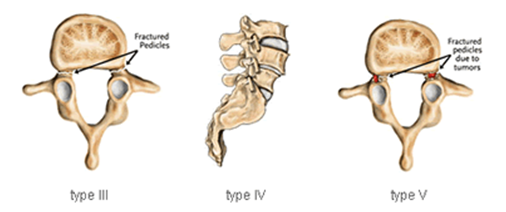
Type III
Type III is a degenerative spondylolisthesis, and occurs as a result of arthritis of the lumbar facet joints. The alteration in these joints can allow forward or backward vertebral displacement. This type of spondylolisthesis is most often seen in older patients. In type III degenerative spondylolisthesis there is no pars defect and the vertebral slippage is never greater than 30%.
Type IV
Type IV is traumatic spondylolisthesis and is associated with acute fracture of a posterior element (pedicle, lamina or facets) other than the pars interarticularis.
Type V
Type V is pathological spondylolisthesis. This occurs because of a structural weakness of the bone secondary to a disease process such as a tumour or other bone diseases.
Causes
Spondylolisthesis is most common in the lumbar area. In children this normally occurs between the fifth lumbar vertebra and the first sacral vertebra and is often due to a congenital malformation of that region of the spine. In adults, the most common cause is degenerative disease (like arthritis) and the slip usually occurs between the fourth and fifth lumbar vertebrae.
Other causes of spondylolisthesis include stress (caused by repetitive hyperextension of the back, commonly seen in gymnasts), and traumatic fractures. Spondylolisthesis may occasionally be associated with bone diseases.
Symptoms
Symptoms of spondylolisthesis can include:
- Increased lordosis (sway back)
- Lower back pain
- Localised tenderness over the spine just above the pelvis
- Pain in thighs
- Pain in buttocks
- Tight hamstrings
- Stiffness in back
- Nerve root signs (leg weakness or changes in sensation) may result from pressure on nerve roots and may cause pain radiating down the legs
Diagnostic tests
- X-ray of the spine – demonstrates malalignment of lumbar vertebrae and possible defects in the bone.
- Straight leg raise – may be uncomfortable or painful due to tight hamstrings
Treatment
Treatment varies depending on the severity of the symptoms of the spondylolisthesis. Most patients require only strengthening and stretching exercises combined with activity modification (avoiding hyperextension of the back and contact sport). Some practitioners also use a rigid brace. Only 10% of spondylolisthesis requires surgery overall.
For cases with severe pain not responding to therapy or if the slip is severe or there are neuralgic changes, the slipping vertebra can be surgically fused. Use of a brace or body cast may be part of treatment after surgical correction of the defect.
Prognosis
Conservative therapy for mild spondylolisthesis is successful in about 80% of cases. When necessary, surgery produces satisfactory results in 85-90% of people with severe, painful spondylolisthesis.